|
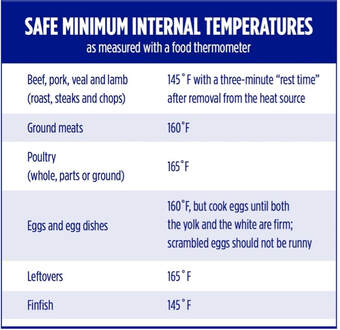
Thanksgiving is quickly approaching which means more time in the kitchen and around the table with family and friends. According to the U.S. Centers for Disease Control and Prevention, one in every six Americans becomes ill each year from consuming contaminated foods or beverages. Therefore, food safety should always be a priority and the holidays are no exception. The good news is you can protect your family and friends from foodborne illness by taking a few smart steps in your kitchen from the Partnership for Food Safety Education “Fight BAC” initiative: clean, separate, cook and chill. There is no better time than now to make sure you’re using proper kitchen safety techniques at holiday parties and meals. PREPARATION Clean Before preparing food, wash your hands thoroughly with soap and water and cover cuts and scrapes with bandages to avoid contamination. When creating holiday dishes with fresh fruits and vegetables, first wash them well under plain running water. It’s not necessary to use soap or a produce wash. The Food and Drug Administration recommends rinsing produce before you peel it, so dirt and bacteria aren’t transferred from the knife onto the fruit or vegetable. You can scrub firm produce like melons and cucumbers with a clean vegetable brush. Also make sure to wash cutting boards, utensils, and counters with hot soapy water between preparing different types of food items. Separate To avoid cross-contamination, cooked and raw foods should be prepared in separate areas on different cutting boards and plates to avoid possible cross contamination with bacteria between foods. For example, fruit or vegetable salads and raw meats should be sliced at another time and separate counter and cutting board, which are washed well between each food’s preparation. Chill Promptly refrigerate or freeze any meat, poultry, eggs, and other perishable foods after grocery shopping. Never let raw meat, poultry, eggs, cooked food or cut fresh fruits or vegetables sit at room temperature for more than two hours before refrigerating or freezing. Do not defrost food, such as your turkey, at room temperature rather, defrost food in the refrigerator, in cold water or in the microwave. If you are using a frozen turkey, keep it frozen until you are ready to thaw. Then, thaw it in the refrigerator, allowing 24 hours of thawing time for every 4 - 5 pounds of turkey. If you choose to thaw your turkey in cold water in a sink, allow about 30 minutes for every pound and change the water every 30 minutes to keep it cool. Don’t forget to cook food thawed in cold water or the microwave immediately. COOKING Additional food safety steps can be taken while cooking and cleaning holiday dishes and utensils. Use different clean utensils for each food item. To avoid bacteria growth, place your holiday turkey immediately into the oven after stuffing and cook it until the center of the turkey reaches at least 165°F. Make sure to cook food to the proper temperature to kill harmful bacteria. Use a food thermometer to check the temperature of cooked meat, poultry and egg dishes as listed in the chart below. Also, be sure to remove and cook the turkey giblets separately. Don’t leave them in the bird. Any utensils used while cooking should be washed in hot water before using them again. STORING LEFTOVERS
Holiday leftovers provide a wonderful way to enjoy holiday favorites a little longer. After eating your meal, slow the growth of harmful bacteria by refrigerating foods quickly. Store your leftovers in the refrigerator or freezer within two hours of being prepared. The best way to store leftover turkey and dressing is in sealed air-tight containers in the refrigerator or freezer. Food can be stored in the refrigerator for 3 - 4 days and in the freezer for 2 - 6 months. Divide large amounts of leftovers into shallow containers for quicker cooling in the refrigerator. A healthy holiday season is a happier holiday season. By using these food safety tips, you will be armed with the tools to stay safe in the kitchen and decrease your risk for food-borne illness. For more information on holiday food safety, check the U.S. Department of Agriculture and Food and Drug Administration websites by searching on “Holiday Food Safety USDA and FDA.” Thanks to Emily Kolasheski, a senior dietetics student at Texas A&M University and my mentee in the Texas A&M/University of North Florida RD Mentorship Program this year, for her assistance with this blog.
0 Comments
 As I was thinking about writing a blog on monosodium glutamate or MSG, I first tried to come up with a snappy title. Fond of using acronyms, I pondered over the letters MSG to come up with one that would be catchy and convey my purpose in discussing it. First, looking at it from the negative perception MSG has had for years, I considered “Misperceptions Slander Gibberish” or “Myths Should Go.” On the flip side, I thought of “More Savory Grub” or “Making Seasoning Great,” because MSG truly enhances the flavor of food. But in the end, I landed on “The Real Truth about MSG: Myths, Science, Guidance.” Using this theme, I’ll lay out the MSG myths and misperceptions often heralded in the headlines, counter those with the scientific facts and conclude with ways to use MSG to create delicious dishes you’ll love to eat. While “No MSG” never reached the fever pitch of no-high fructose corn syrup, gluten-free or non-GMO, it has nevertheless negatively permeated the consciousness of Americans for over five decades. Discovered over 100 years ago, MSG is a flavor enhancer that is a staple in Asian kitchens like salt and pepper are here. But over the years, it has garnered an unfair share of damaging headlines like “Chinese Restaurant Syndrome: What you need to know,” “4 Signs MSG is Poisoning Your Body,” and “MSG is Dangerous – The Science is In.” But once you really get to KNOW MSG, you’ll never say NO MSG again! Myths So how did MSG end up on the “public enemy” food ingredient list? It all started in 1968 when a U.S. Chinese physician wrote a letter to the editor published in the prestigious New England Journal of Medicine. He noted that when he ate in a Chinese restaurant in the U.S., he experienced symptoms which usually began 15 to 20 minutes after he ate the first dish and lasted for about 2 hours without any hangover effect. The most prominent symptoms were numbness at the back of the neck, gradually spreading to both arms and the back, general weakness and palpitation similar to, but milder, than those he had from a sensitivity to aspirin. He heard complaints of the same symptoms from Chinese friends, both medical and nonmedical people. In the article, he theorized that these symptoms might be caused by the cooking wine, monosodium glutamate or the high sodium content of the Chinese food. He did not single out one possible cause over another, but MSG is what caught the attention of the media. In response, researchers conducted studies in mice, injecting large amounts of MSG directly into their brain and abdomen, which produced negative effects. This led to further questions about MSG’s safety, despite its use in the U.S. food supply for over 50 years. But these studies are not relevant to MSG consumption in humans because, as you will read below, there is no way MSG can actually enter the blood stream and travel to the brain or abdomen unless it is injected! And who’s going to do that? Science MSG - monosodium glutamate - is a salt combining sodium and glutamic acid, a non-essential amino acid. When glutamic acid loses a hydrogen from its structure, it becomes glutamate. In the body, glutamic acid almost always exists as glutamate. When MSG is exposed to liquid, whether in a recipe combined with liquid or in saliva, the sodium separates from the glutamate. Therefore, it cannot and does not enter the body as MSG but as glutamate and sodium separately. And these two components are not reformed into MSG in the body. Glutamate is what provides “umami” to food, a savory taste that enhances the flavor of dishes. The discovery of the umami taste receptor on the tongue in 2002 led to the designation of umami as the fifth basic taste along with sweet, salty, sour and bitter. Umami is the distinctive flavor you taste in foods like tomatoes, mushrooms, aged cheeses and meats. People have eaten glutamate-rich foods throughout history long before MSG was around. Infants even consume up to 145 mg/day of free glutamate in breast milk. Here are some common foods with the amount of glutamate they contain. 3 oz. cured ham 285 mg 1/2 cup tomato 220 mg 1 Tbs. soy sauce 65 – 200 mg 1 Tbs. Roquefort cheese 110 mg 1/2 cup corn 90 mg mg. 1 Tbs. Parmesan cheese 60 – 85 mg 1/2 cup broccoli 80 mg 1/2 cup green peas 80 mg 1 cup Napa cabbage 75 mg 1/2 cup dried shitake mushrooms 15 mg The body is unable to tell the difference between glutamate in MSG and free glutamate that comes from proteins in food. Our bodies metabolize them both in the same way. The average adult consumes approximately 13 grams of glutamate/day from protein in food, while intake of added MSG is about 0.55 grams/day. You would have to eat 3 mg. of MSG all at one time without any food in order to produce the mild symptoms that have been seen in only a small number of people. Safety Numerous studies attest to the safety of MSG. In one a panel of experts evaluated the metabolic and safety aspects of monosodium glutamate and concluded that general use of glutamate salts, like MSG, as a food additive can be regarded as harmless for the whole population. (1) In another, researchers found that human studies failed to verify that MSG is a cause of "Chinese Restaurant Syndrome" or other individual intolerances. (2) And a third stated that the reported negative health effects of MSG are not relevant because they are based on excessive amounts that people do not normally consume. (3) MSG’s safety has also been affirmed by regulatory agencies. According to Food Standards Australia New Zealand, there is no convincing evidence that MSG is a significant factor in causing reactions resulting in severe illness or death. (4) Likewise, the U.S. Food and Drug Administration states it has never been able to confirm that MSG has caused effects such as headache and nausea. (5) Guidance (and Goodness!) One of the great benefits of MSG is its potential to lower sodium in dishes without compromising flavor. (6) One study demonstrated that it could potentially reduce the intake of sodium by approximately 3% in the population overall and by 7% among consumers of products in which glutamates could replace salt. (7) And a review of seven studies on the acceptability of low salt products found MSG to be the best replacement for salt to maintain the pleasantness, saltiness, familiarity and taste intensity while reducing health problems linked to a higher sodium consumption. (8) In contrast to table salt with 2300 mg. sodium/teaspoon, MSG has just 800 mg. sodium per teaspoon. Even better, it can replace up to 61% of the salt in a dish without compromising flavor. For instance, 1/2 teaspoon of MSG (400 mg.) can enhance the flavor of a 1 pound of meat (4 servings) or 4-6 servings of vegetables, casserole or soup for just 100 mg. sodium per serving. Replacing half of the salt in your salt shaker with MSG reduces the sodium in the mixture by about 40%. There is even a product now available that is half MSG and half salt. Here are tips for using MSG in a variety of dishes from Ajinomoto, a company that produces MSG.
For additional recipes and information about MSG, check out their website, Facebook page or @know_msg on Instagram. And if you’d like to give MSG a try, some brands to look for are Accent, Ajinomoto MSG and McCormick Culinary MSG. References
 By Marissa Gregurek, Dietetic Intern, University of Oklahoma Marissa Gregurek was the 2020 recipient of the University of Oklahoma Mary Green Lovelace Endowed Scholarship. I established this fund with the OU's College of Allied Health Nutritional Sciences Department in 2018 for a student working toward becoming a registered dietitian nutritionist. One of the application requirements is a 500-word essay addressing how registered dietitian nutritionists can effectively communicate the role of modern agriculture and the food industry in providing a safe and adequate supply of nutrient-rich food for people in the U.S. and around the world. This blog is Marissa’s essay that so eloquently articulated my philosophy on this topic. Marissa also completed a 1-week nutrition communications rotation with me in March 2021. Farm to table. Although this simple phrase has exploded as a popular marketing term, it also innately involves nutrition and those who study it. Dietitians form an essential link in our food supply, ideally connecting consumers to knowledge about where food comes from and how it affects their health. Growing up in rural Texas, agriculture was a part of my life from an early age. Although in college I majored in biomedical science, I took much more interest in the animal science classes I was pursuing for my minor. I eagerly learned about animal husbandry, meat science, and food production, topics which seemed much more practical and important than the abstract concepts I struggled with in physics and organic chemistry. As I begin a career in dietetics, my background in agriculture provides a sturdy ground on which to stand, as an advocate for farmers and consumers, and for nutrition strategies that benefit both. In particular, I seek to dispel some of the nutrition myths surrounding the livestock industry. While plant-based foods offer an amazing array of phytochemicals and antioxidants, meat also helps comprise a balanced diet and doesn’t deserve the sense of “evil” often associated with it. I hope to communicate that ranchers who administer vaccines and antibiotics to their herds are actually protecting our food supply from viruses and disease. If unchecked, these pathogens could cause significant animal suffering and lead to shortages that increase food insecurity. I would explain that livestock help us utilize the parts of crops that humans can’t eat, like soybean hulls, corn stalks, and brewers’ grains, to make our food system more efficient. Additionally, grazing livestock in many areas where crops won’t grow helps convert non arable land into an energy dense, high protein food source. I would advise that meat, dairy, and poultry offer powerful benefits in terms of iron, Vitamin B12, calcium, zinc, and protein, and that these nutrients are more bioavailable from foods than from supplement sources. I hope to counter fears about eggs being a dangerous cholesterol source, instead encouraging that they can serve as a healthy, versatile protein packed with nutrients. I plan to use my knowledge of meat science to help those in need of low-fat diets identify leaner grades and cuts of meat. Finally, I can use my food production expertise to offer meaningful nutrition recommendations to those clients following Kosher, Halal, or other dietary practices. While science doesn’t support eating meat for every meal, complete abstinence from these foods isn’t mandated either. I hope to empower clients to make informed decisions about animal products based on the facts and not on fears. Behind me are the hard-working farmers and ranchers that I grew up with in Central Texas, who strive to create a safe and bountiful food supply. Before me are the clients and patients that, as a future dietitian, I plan to counsel on the path to healthier eating. I hope to do justice to both.  I was thrilled when the new edition of DASH Diet for Dummies came out and I actually had it in my hands! I received a complimentary copy from the publisher and was eager to post a review on Amazon. Imagine my surprise when I was blocked from writing a review, not only on my own account but also on my husband’s Amazon Prime account. Both times I received a message, “We apologize but Amazon is not accepting reviews on this product from this account. If you would like to contact us about this decision, please email community-help@amazon.com.” I did email “community help” but they never responded. Next I called and spoke with an Amazon customer service rep who told me that someone would call me the next day to discuss it. No one ever called. Finally, I decided to outsmart Amazon and create a new account using an alternate email address. Once I did that, I discovered I had to spend $50 before I could review a product. So I bought a Valentine’s Day present for my husband along with a copy of DASH Diet for Dummies, Second Edition so I would have a “verified purchase” when I wrote my review. Of course, this did not qualify me to immediately post a review. I had to wait until several days after the order was delivered before I could do that. But once they allowed me to, I was thwarted once again. I received this message: “Thank you for submitting a customer review on Amazon. After carefully reviewing your submission, your review could not be posted to the website. While we appreciate your time and comments, reviews must adhere to the following guidelines: Amazon Community Guidelines.” Frustrated but undeterred, I decided to circumvent Amazon and post my review as a blog and promote it widely on social media! So here it is, in all its Amazon “illegal” glory! As nutrition communications consultant, I daily translate technical scientific nutrition information into practical, consumer-friendly messages to help folks enjoy food without fear. The authors of this new edition of DASH Diet for Dummies have successfully accomplished this. They explain the science of high blood pressure in clear-cut, straightforward terms; provide practical, creative ways to make the DASH Diet a part of everyday life for busy people and transform the guidelines into delicious recipes that are easy to prepare. Having known Cindy Kleckner for over 40 years, as she transitioned her career from clinical practice to culinary nutrition, I’ve seen firsthand the love, passion, creativity and care she puts into each and every dish she creates for family, friends and her many culinary presentations. It is truly her calling. In addition, Rosanne Rust and I have worked together with many of the same clients for over 10 years and share a fervor for promoting accurate food and nutrition information, as the authors have done in this book. Finally, their colleague, Dr. Sarah Samaan successfully breaks down the medical perspective on high blood pressure in a practical way. I highly recommend this book not only for people looking for nutrition guidance to manage blood pressure but for anyone interested in an eating plan that provides a balanced variety of delicious foods to promote health and nutrition. It’s DASH: Delicious And So Healthy! If you'd like to order a copy, here are links to do so: Target Walmart Wylie Publishers  I am in my second year as an invited Produce for Better Health Foundation volunteer Fruit and Vegetable Ambassador. In this role, I promote the fun, flavor and benefits of produce in a variety of ways every month. This is my January contribution for which I received no financial compensation. For many folks, kicking off a new year means making resolutions, often admirable but frequently difficult to maintain. In fact, just 40% of us stick with them for 6 months and a mere 19% for 2 years according to University of Scranton psychology professor John Norcross, PhD, who has studied compliance to New Year’s resolutions, One strategy that may help is making resolutions more achievable. Aim for evolutionary change, not revolutionary change. Making small steps will add up to big changes over time. This makes them less daunting. As a registered dietitian nutritionist, one of my goals is to find ways to encourage people to eat well-balanced, nutrient-rich meals and snacks they will enjoy. We all know eating fruits and vegetables is good for us but it’s still where most people fall short. And this is confirmed in the new 2020 – 2025 Dietary Guidelines for Americans, which say 75% of Americans are not eating enough fruits and veggies. But how can we boost fruit and veggies in our meals so it’s less of a challenge and more of an easy and natural part of everyday life? First, don’t think of them just for their health benefits but focus on the fun, flavor and fitness potential they also provide. Then find easy, tasty ways to do that. While the Dietary Guidelines recommend 2 ½ cups of veggies and 1 ½ cups of fruit a day, you don’t need to achieve this the first day. Instead, start slowly and make just one change each month over the next year. Rather than resolutions that go by the wayside, create “plant-entions” that are easy to stick with. Here’s a month-by-month guide with ideas. January: Add a fruit or veggie at breakfast. This can be as easy as drinking a 6-ounces of 100% orange, grapefruit or tomato juice or adding banana, raisins or another fruit to your cereal. February: Add a fruit or veggie at lunch. Layer a sandwich with lettuce and tomato or add sliced pears to a grilled cheese sandwich, opt for a small salad with your meal or grab a piece of fresh fruit for dessert. March: Add a fruit or veggie at dinner. Double up your veggie intake by topping a baked potato with steamed veggies and cheese or a heaping helping of salsa. Or how about a green salad with fresh or canned peaches or pineapples slices topped with cottage cheese? April: Eat a fruit or veggie for a snack. Keep small boxes of raisins in your desk drawer at work or stuff celery sticks with spreadable cheese or peanut butter. May: Sneak in a fruit or veggie at breakfast. Scrambling up some eggs? Stir in canned diced tomatoes and green chilies for added color and flavor. Or spread your English muffin, bagel or toast with mashed avocado in place of cream cheese or jelly. June: Sneak in a fruit or veggie at lunch. Add diced celery or apple to tuna or chicken salad or zap a half cup of frozen blueberries or other frozen fruit in the microwave at 50% power for 45 seconds and combine with yogurt. July: Sneak in fruits and veggies at dinner. Cooking chicken or steak on the grill? Cut the meat into chunks and thread on a skewer for kabobs with cherry tomatoes, mushrooms, squash, pineapple, bell pepper and more. Or pour your spaghetti sauce over spiralized veggies. Don’t have a spiralizer or want to go to the trouble? No problem. You can buy frozen spiralized zucchini and carrots that cook in the microwave in minutes. August: Sneak in fruits and veggies at snacks. Dip tortilla chips, sliced carrots or cucumbers in a vegetable-based dip like guacamole, salsa or hummus. Or instead of a package of nuts, make your own snack bags with nuts plus raisins or dried cranberries. September: Add fruits and veggies when dining out. Produce is not always front and center on restaurant menus. Whether it’s a casual cafe, ritzy restaurant or the fast food drive-through, you can find options to add to your meal. Add a side salad to your meal if that’s a choice. Also, peruse the sides on the menu and select a green or yellow veggie to go with your entree. Finally, look for a dessert with fruit as an ingredient or ask for a fruit plate if it’s not on the menu. October: Boost the taste appeal of fall produce. Fall brings an array of delicious vegetables like Brussels sprouts, acorn and butternut squash, turnips and carrots. To truly bring out their natural sweetness and flavor, try roasting them in the oven. This recipe for Pan Roasted Root Vegetables can be used with other veggies, too. November: Add fruits and veggies to beverages. Bored with plain old water? Jazz it up a bit by making a juice spritzer with half juice and half sparkling water. For a more substantial snack or a quick breakfast on-the-go, whip up a smoothie with yogurt, banana, frozen mango and orange juice. And for holiday drinks, try a Cranberry Sour or Holiday Rosé. December: Boost fruits and veggies in holiday meals. From appetizers like Mini Quiches to Apple Cranberry Stuffing, Mandarins & Beet Holiday Salad, Herb-Topped Beef with Roasted Cauliflower and Apple Pie, there’s not an item on the menu that can’t include fruits and veggies! Remember that life is a marathon, not a sprint. Change takes time and so do results. By taking small, simple steps each month, you’ll be sure to have a happy, healthy 2021! For more information plus fun and flavorful ways to add more fruits and veggies to your meals and snacks, check out https://fruitsandveggies.org  Even with anxiety and stress already high due to the current COVID-19 pandemic, the Environmental Working Group (EWG) still found it necessary to release its annual Dirty Dozen list yesterday. It lists the 12 fruits vegetables that allegedly have the highest levels of pesticide residues. But it’s actually just a thinly veiled attempt to create fear of conventionally grown produce and steer folks to buying expensive, organic produce. NEWS FLASH: organic farmers can and do use pesticides, natural and approved synthetic ones. FACT: pesticide residues on all produce – organic and conventional - are very low, if measurable at all. Yesterday’s new list was identical to last year’s, same foods in the same order. While coronavirus news garners the lion’s share of headlines today, I did find a few inflammatory Dirty Dozen headlines on the second and third page of a Google search, “Strawberries Top the EWG's 2020 Dirty Dozen List” and “These 12 Foods Are Most Likely to Carry Pesticide Residue.” This one was actually a bit surprising: “Here are the ‘dirty dozen’ fruit and vegetables laced with legal pesticides — even organics have traces.” Key words here are “traces” and “organics.” So let’s take a closer look beyond the sensational headlines for a few things you need to keep in mind. First, pesticide residues on conventionally grown produce are tested annually by the United States Department of Agriculture (USDA), with the results published in their Pesticide Data Program Annual Summary. In the most recent 2018 report, USDA found that “more than 99% of the samples tested had pesticide residues well below benchmark levels established by the Environmental Protection Agency (EPA). The EPA sets these benchmarks to ensure that pesticide residues remain at levels that EPA has determined to be safe in or on foods for human consumption.” And 48% of the samples tested had no detectable pesticide residue at all. Second, as I previously mentioned and contrary to popular belief, organic farmers do use pesticides. Many are natural pesticides (but still kill insects and weeds) like sulfur, bicarbonate, copper and vinegar but also include synthetic pesticides approved for organic use. While organic produce is not regularly tested for pesticide residues, in 2010 the National Organic Program worked with the USDA to evaluate pesticide residues on 571 domestic and foreign fruit and vegetable samples bearing the USDA organic seal. The report revealed that 96% of the samples tested met the USDA organic regulations, with 57% showing no detectable residues and 39% with residues less than 5% of the EPA allowable level. The fact is you have nothing to fear from eating any type of produce. All pesticide residues on fruits and vegetables, whether organically or conventionally grown, are extremely low and well below any level that could put you at risk. And according to University of California Berkeley Emeritus Professor of Biochemistry and Molecular Biology, Dr. Bruce Ames, 99.99% of the pesticides we eat are naturally present in plants to ward off insects and other predators. That means only 0.01% of ingested pesticides are synthetic. So how does the Environmental Working Group come up with the data in its report that leads consumers to assume their produce is laden with pesticide residues? Believe it or not, they use the data in the USDA report mentioned above! Unfortunately, they misrepresent the data. How? They rank the fruits and vegetables in order of the pesticide residues found, from the highest to lowest amounts. Then they label the top twelve as “The Dirty Dozen.” But, as I explained earlier, the residue levels are extremely low and 99% of the samples tested fell well below the tolerance levels and 48% had no detectable pesticide residues. And two PhD toxicologists debunked the methodology the EWG uses to create this list in their research article in the Journal of Toxicology. To put the EWG’s method into perspective, consider this comparison to National Merit Scholars. Most of us know these are very smart high school students who scored highly on the qualifying PSAT/NMSQT exam. So, imagine taking the list of National Merit Scholars for this year and ranking them according to their exam scores from highest to lowest and then taking the bottom twelve and calling them “The Dumbest Dozen.” If you look deep into the EWG website you’ll find this disclaimer, “The health benefits of a diet rich in fruits and vegetables outweigh the risks of pesticide exposure. Eating conventionally grown produce is far better than skipping fruits and vegetables.” Of course, this statement never makes it into the articles with the sensational headlines. The EWG is not a research or academic institution with independent scientists. It is an activist group with some funding from the organic industry. In a survey of the scientist members of the Society of Toxicology, 79% say EWG overstates the health risk of chemicals. According to a 2019 survey from the Alliance for Food and Farming (AFF), there was almost unanimous agreement among registered dietitians that it is important for consumers to know that conventionally grown produce is safe because not all people can afford to buy organic. They also believe that inaccurate, fear-based messages cause consumers to question whether eating conventionally-grown fruits and vegetables is safe. Want to find out how many servings of a particular fruit or vegetable you could eat and still not have any adverse effects from pesticide residues? Check out the Pesticide Residue Calculator on the Safe Fruits and Veggies website. It turns out an adult woman would have to eat 453 servings of strawberries, 773 servings of spinach, 3,344 servings of organic lettuce or 4159 servings of conventional lettuce in one day without any effect, even if they had the highest pesticide residues level ever recorded by USDA for these foods. If you’re still concerned, keep in mind that you should always wash your fruits and vegetables. Produce is grown in fields with soil. Many hands touch the produce from the time it leaves the field until it gets into your kitchen. From farmworkers to produce packers to supermarket employees to other customers, many bacteria-laden hands have landed on your fruits and veggies. While the main reason to wash it is to get rid of dirt and bacteria, it can also eliminate any tiny amounts of pesticide residues if they are even present. Over 90% of people in the U.S. don’t eat enough fruits and vegetables so we should not be doing anything to discourage folks from enjoying any type of produce they like to eat, whether it is conventional, organic, fresh, frozen, canned, dried or juice. They all count toward your daily recommended fruit and veggie intake, are nutrient-rich and make you look and feel good. So, relax and enjoy the taste and fun of filling half your plate with fruits and vegetables. And for more information about fruits and vegetables and delicious ways to enjoy them, check out the Produce for Better Health Have A Plant website.  Growing up, orange juice was a staple on our breakfast table. And juice has continued to be part of my morning routine ever since. A 6-oz. glass of OJ supplies 100% of the daily recommended intake for vitamin C along with an array of other nutrients, all for just 80 calories. And it’s a quick and easy way to consume at least a third of your daily quota of fruit. So imagine my surprise – and chagrin – when I learned that parents are being warned against serving fruit juice to their kids based on claims that juice is loaded with sugar and causes childhood obesity. A recent Wall Street Journal article actually characterized juice as a “gateway drink” to sodas and other sugar-sweetened beverages. Whoa! Are we seriously comparing fruit juice to a drug?? That’s definitely going too far in my book and sadly misjudges juice and its positive contributions to kids’ – and everyone’s – nutrient intake. As a result of the negative press, many parents are forgoing juice altogether or diluting it with water. And some enterprising companies have jumped on the bandwagon by selling watered-down juice at a premium price. Just remember, this dilutes the nutritional contributions of juice by 50% as well. And it seems ironic that while parents are depriving their kids of juice, they’re drinking more of it themselves! The last decade has brought a boon in the sale of home juicers and a rise in juice and smoothie bars. But no one is saying the fruit from which juice is made contributes to negative outcomes. As one of the 16 volunteer Produce for Better Health Foundation Fruit and Vegetable Ambassadors, we promote all five forms of produce: fresh, frozen, canned, dried and juice. So let’s explore more about the positive attributes of juice and dispel some myths. Fruit Juice is Not Soda In the past three decades fruit juice has gone from a perfectly acceptable breakfast beverage to one lumped in the same category as sugar-sweetened beverages like soda. A recent study based on self-reported sugary drink consumption, grouped soda and fruit-flavored drinks together with 100% fruit juice (but not sweetened tea) and concluded that they caused an increase in deaths. This analysis had several shortcomings, some acknowledged by the researchers: the number of participants who died during the relatively short follow-up period was small; the causes of death were not identified; soda consumption was self-reported, which is often underreported; results were based on 12-ounce portions, which is larger than usual for juice; and they did not estimate intake of all types of sugar-sweetened beverages, including sweetened tea. While sugar content of soda and 100% juice may be similar, the comparison stops there. Fruit juice is a source of essential nutrients while sugar-sweetened beverages such as soda or fruit-flavored drinks provide no other nutrients besides sugar. And, according to a new study, there is no evidence to support claims that fruit juice consumption is linked to childhood weight gain or metabolic effects. Another recent study found similar results: children who drank more milk, 100% juice and water and less soda had better quality diets and giving up juice was not linked with lower body weights. Fruit Juice is Nutrition-Packed Juice is an easy way for children to obtain one or two fruit servings each day along with the key nutrients it contains. Juice delivers vitamins, minerals and phytonutrients important for good health including vitamins A, C and folic acid along with the minerals magnesium and potassium. In addition, those who drink fruit juice have a more nutrient-rich diet overall as well as a lower intake of added sugars, saturated fat and sodium. Juice is also a great way to help meet daily fluid needs and stay hydrated. But recommendations to limit juice can have unintended nutritional consequences. As people have consumed less fruit juice over the last 30 years, they have not replaced it with more whole fruit, so children and adults may not meet their daily recommendation for fruit intake. Consider Juice as Part of the Total Diet When you only look at individual foods or beverages in your daily meals, you may fail to see the big picture of how all foods and beverages work together to create a nutritionally adequate intake and influence your weight and health. Juice is only one component of your diet, so to claim that juice leads to obesity or other problems is misleading. There are many contributing factors and no single food or ingredient is responsible for negative effects. Simple “one-size-fits-all” solutions are not the answer. Including both 100% juice and whole fruit with meals and snacks is the best way to meet the daily recommended servings of fruit. How much do we need to eat? For children 1 – 6 years old, a total of 1 cup of fruit and juice each day is recommended and for those 7 – 12, 1½ cups should be consumed. Anyone 13 or older needs 2 cups of fruit over the course of the day, including juice. With 75% of Americans not consuming enough fruit, we should not be doing anything to discourage folks from eating any kind of fruit. That’s why the 2015-2020 Dietary Guidelines for Americans recommend increasing fruit in all forms, including 100% juice. According to the Guidelines, one cup of 100% fruit juice counts as 1 cup of fruit. And while they recommend at least half of the recommended amount of fruits be whole fruit (fresh, frozen, canned or dried), that means up to half of daily fruit intake may come from 100% juice. So stop worrying…and put juice back in your shopping cart and on your table for the entire family! *A special thanks to Texas Health Resources Presbyterian Hospital Dallas Dietetic Intern, McKenzie Hicks, for her assistance with this blog.  This blog was written in a paid partnership with the American Frozen Food Institute. However, the opinions expressed represent my personal views on food safety, nutrition and healthy eating. Before the proverbial ink was dry on my listeria and lettuce blog, yet another scary headline emerged that appeared to question the safety of eating frozen produce. I am beginning to think there is a conspiracy in the media to discourage people from eating fruits and vegetables. And as a registered dietitian this is disappointing as my colleagues and I are doing everything we can to encourage folks to eat more produce. That’s because only one in 10 people in the U.S. consumes the recommended daily servings of fruits and veggies. Packed with nutrition, I promote all forms of fruits and vegetables to make it easy for people to eat more: fresh, frozen, canned, dried and juice. First, let me share all the reasons I love frozen fruit.
Frozen food manufacturers are very diligent in making sure fruit is safely processed and packaged to prevent foodborne illnesses. Frozen fruit is thoroughly cleaned, washed and flash frozen within hours of being harvested. Once frozen, no bacteria can grow but, contrary to popular belief, freezing does not kill bacteria or viruses. That’s why so much care is taken to clean the fruit well before it is frozen, just like we wash fresh fruit at home that is purchased at a supermarket or farmers’ market. So back to the scary headlines. Last week the Washington Post reported on a new U.S. Food and Drug Administration (FDA) program that is testing frozen berries for hepatitis A virus and norovirus. According to the FDA website, in 2019 and 2020, the agency will collect and test samples of U.S. grown and imported frozen packaged strawberries, raspberries and blackberries from processors, distribution centers, warehouses and supermarkets. If they find hepatitis A virus or norovirus, FDA will notify and work with the company to take action to protect the public health, such as issuing public warnings or instituting a product recall. (1) The Post article stated that since the inspections began in May, FDA has recalled one brand of a frozen blackberry product and one of a blended berry product that were found to contain parts of the hepatitis A virus. While the FDA advised consumers not to eat and to throw away the specific berry products identified, they noted that no cases of hepatitis A had been linked to them. (2) Why would berries contain viruses or bacteria? They may become contaminated if handled by an infected worker who does not wash his or her hands properly or if the berries are exposed to a contaminated surface or agricultural water. As I mentioned earlier, bacteria, viruses and microorganisms can survive at low temperatures, including freezing. That’s why the industry is so diligent in its food safety practices. Foodborne illness is a serious issue so we are very fortunate in the U.S. to have government agencies like the FDA, U.S. Department of Agriculture (USDA) and the Centers for Disease Control and Prevention (CDC) who are vigilant in setting standards and monitoring the safety of our food so that we have the safest food supply in the world. The Post article also quotes Dr. Donald W. Schaffner a food science professor at Rutgers University who states that FDA tests for the DNA of the two viruses and the recall do not mean the berries contained the whole, live hepatitis A virus that causes illness. He goes on to say that he is not changing his berry eating habits as a result of this report because they are “safe, healthy foods” and “We want people to eat more fruit and vegetables.” And the Academy of Nutrition and Dietetics agrees. An article on their website by registered dietitian nutritionist Esther Ellis says, "Frozen foods are an affordable way to get your daily dose of fruits and vegetables. In fact, families who incorporate frozen foods into their normal routine may have better diet quality.” References:
 Those who follow my blog and social media know I’m passionate about promoting fact-based food and nutrition information to help people “eat beyond the headlines” and enjoy a variety of nutrient-rich foods. Most of the time those scary headlines are a result of a study misrepresented and sensationalized in the media or an activist group with an agenda fostering fear about perfectly safe foods or ingredients. But the headlines that appeared in the news this past week evoke fear of food for a different reason and that’s food safety. The latest headlines are a result of a Consumer Reports investigation of 284 samples of bagged and loose lettuce and other leafy greens from supermarkets that found six (2%) contained listeria. Listeria monocytogenes is a bacteria that causes the foodborne illness listeriosis especially in high-income, industrialized countries. It is widespread in the environment. According to the U.S. Food and Drug Administration (FDA), compared to other foodborne illnesses, listeriosis is rare but very serious. Healthy children and adults occasionally get listeriosis, but seldom become seriously ill. People with weakened immune systems, pregnant women and the elderly, however, are at greater risk of a more severe form of listeriosis. (1) The report quotes the Centers for Disease Control and Prevention’s (CDC) medical officer, Karen Wong, M.D., as saying, “It is rare for healthy adults to get sick with listeria infection.” SPOILER ALERT: This report does NOT advise people to stop eating lettuce and leafy greens. Nor does the report mean that leafy greens are riskier than any other foods – despite the scary headline. In fact, the report notes that listeria is usually associated with deli meats, hot dogs, soft cheeses and sprouts. They also state that the “study represents a snapshot of the market and was not large enough to draw conclusions about the safety of specific brands or retailers.” Keep reading for more context. Food Safety Facts Listeria is commonly found in many food items, not just leafy greens. If you check the FDA’s website you will see that several were involved in recent recalls due the detection of listeria. These included egg, tuna and lobster products in addition to other vegetables like squash and cauliflower. We are fortunate in the U.S. to have the safest food supply in the world. Our government and its agencies like the U.S. Department of Agriculture (USDA), Food and Drug Administration (FDA) and Environmental Protection Agency (EPA) have regulations and programs that ensure those who grow, process and distribute our food are following high standards of safety and sanitation. There are other voluntary organizations that set additional standards and conduct testing of foods and farms to further ensure safety. But no system is perfect and at times we do have outbreaks that compromise the safety of a food for a short period of time. But, again, the government and its departments are quick to evaluate the situation and make sure the offending products are removed from our food supply until the problem is resolved. Produce Perks As registered dietitians, my colleagues and I are concerned that most folks in our country are not eating enough fruits and vegetables. In fact, only 1 in 10 people consume the recommended amount of produce each day. A just-published study in Critical Reviews in Food Science and Nutrition reviewed nearly 100 studies that looked at the effects of fruits and vegetables on a variety of diseases. Their findings: eating at least five servings of fruits and vegetables every day can drastically reduce the risk of heart disease, protect us from certain forms of cancer and promote eye and bone health, among other benefits. (2) So anything that prevents people from eating fruits and vegetables is a concern for me, whether it’s from scary headlines that promote misinformation or real food safety issues. Putting these headlines in perspective is among the roles I play as a nutrition communications specialist. To this end, I have partnered with two organizations to further my efforts. First, I’m one of 16 volunteer Fruit and Vegetable Ambassadors in Action selected by the Produce for Better Health Foundation. Our role is to encourage increased intake of fruits and vegetables, not only for their many health benefits but also because they help you look good, feel good and have more energy. I am also a consultant with the Leafy Greens Marketing Agreement (LGMA), to help spread the word about the safety and nutritional value of leafy greens. LGMA is a program that verifies compliance with the food safety practices of leafy green growers through mandatory government audits. Putting it in Perspective How often does food contaminated with listeria actually result in an illness? The number of foodborne illnesses is extremely small compared to the vast amount of food eaten in the U.S. And when it comes to leafy greens, the chance of becoming ill is much, much less than the risk of dying in a plane crash or being struck by lightning. Yet 1 in 4 people die of heart disease every year in the U.S. (3) And that is a statistic we know can be dramatically improved by eating more fruits and vegetables, including leafy greens like lettuce and spinach. Consumer Reports focused only on lettuce and leafy greens in this new report. Because leafy greens are packed and most often eaten raw, it is not overly surprising that that 2% of the samples tested contained listeria. They did not test other food products or even fresh vegetables to see if they had a similar small number with listeria. And they did not find other bacteria that cause foodborne illness, such as salmonella and E. coli in these 284 samples. In reality, Consumer Reports’ findings are in line with previous ones conducted by U.S. government agencies. A study published in 2017 found listeria monocytogenes in just over one percent of 1,700 raw cut vegetable samples tested from 2010-2013 by USDA and FDA scientists. And this is similar to previously published research, which the fresh produce industry relies on to stay informed and in front of food safety concerns that could affect consumers. The Bottom Line This report does NOT mean leafy greens are riskier than any other foods. And, in my professional opinion, greens deliver much greater health benefits than health risks. I am not, however, suggesting that we should ignore health warnings related to foodborne illness. We certainly should, especially when a government agency issues a recall or consumer advisory, which they have not done so far in this case.. People in vulnerable groups – those with weakened immune systems, the elderly and pregnant women - may want to take additional precautions such as these mentioned in the Consumer Reports article:
Fortunately leafy greens like kale and spinach are delicious and just as nutritious when they are cooked as when eaten raw. The CDC also provides additional suggestions for preventing illness from listeria due to other foods on their website.
 A dietitian friend recently told me a story about one of her nutrition counseling clients. When discussing fruits and vegetables, he told her he only ate organic produce. When she asked why, he replied, “Honestly, I just don’t want to have to wash my produce.” He thought the only reason to wash fruits and vegetables was to remove pesticide residues and he assumed that organic would have none. Much of the fear of pesticide residues on non-organic produce is driven by the Environmental Working Group’s (EWG) annual Dirty Dozen list. This list garners headlines like, “Kale Is One of the Dirtiest Vegetables” and “Are You Eating Pesticide-Laden Produce?” It is a thinly veiled attempt to scare hard-working, cash strapped Americans away from buying conventional fruits and vegetables and instead choosing higher-priced, organic produce. Taking a closer look beyond the sensational headlines, there are a few things you need to keep in mind. First, the main reason to wash fruits and vegetables is to get rid of dirt and bacteria. Produce is grown in fields with soil. Also, just think of the number of hands that have touched your produce from the time it leaves the field until it gets into your kitchen. From farmworkers to produce packers to supermarket employees to other customers, many bacteria laden hands have landed on your fruits and veggies. Second, pesticide residues on conventionally grown produce are tested annually by the United States Department of Agriculture (USDA), with the results published in their Pesticide Data Program Annual Summary. In the most recent 2017 report, USDA found that over 99% of the samples tested had residues well below the tolerances established by the Environmental Protection Agency and, of these, 53% had no detectable pesticide residue at all. And third, contrary to popular belief, organic farmers do use pesticides. Many are natural pesticides (but still kill bugs and weeds) like sulfur, bicarbonate, copper and vinegar but also include synthetic pesticides approved for organic use. While organic produce is not regularly tested for pesticide residues, in 2010 the National Organic Program worked with the USDA to evaluate pesticide residues on 571 domestic and foreign fruit and vegetable samples bearing the USDA organic seal. The report revealed that 96% of the samples tested met the USDA organic regulations, with 57% showing no detectable residues and 39% with residues less than 5% of the EPA allowable level. The fact is you have nothing to fear from eating any type of produce. All pesticide residues on fruits and vegetables, whether organically or conventionally grown, are extremely low and well below any level that could put you at risk. The December 2018 news release from the USDA for their most recent report was headlined, “USDA Releases 2017 Annual Pesticide Data Program Summary, U.S. Food Supply is Among the Safest in the World.” And according to University of California Berkeley Emeritus Professor of Biochemistry and Molecular Biology, Dr. Bruce Ames, 99.99% of the pesticides we eat are naturally present in plants to ward off insects and other predators. That means only 0.01% of ingested pesticides are synthetic. So how does the Environmental Working Group come up with the data in its report that leads consumers to assume their produce is laden with pesticide residues? Believe it or not, they use the data in the USDA report mentioned above! Unfortunately, they misrepresent the data. How? They rank the fruits and vegetables in order of the pesticide residues found, from the highest to lowest amounts. Then they label the top twelve as “The Dirty Dozen.” But, as I explained earlier, the residue levels are extremely low and 99% of the samples tested fell well below the tolerance levels and 53% had no detectable pesticide residues. And not one but two PhD toxicologists have debunked the methodology used by the EWG to create this list in their research article in the Journal of Toxicology. To put the EWG’s method into perspective, consider this comparison to National Merit Scholars. Most of us know these are very smart high school students who scored highly on the qualifying PSAT/NMSQT exam. So, imagine taking the list of National Merit Scholars for this year and ranking them according to their exam scores from highest to lowest and then taking the bottom twelve and calling them “The Dumbest Dozen.” If you look deep into the EWG website you’ll find this disclaimer hidden in the Q&A section, “The health benefits of a diet rich in fruits and vegetables outweigh the risks of pesticide exposure. Eating conventionally grown produce is far better than skipping fruits and vegetables.” Of course, this statement never makes it into the articles with the sensational headlines. The EWG is not a research or academic institution with independent scientists. It is an activist group with some funding from the organic industry. In a survey of the scientist members of the Society of Toxicology, 79% say EWG overstates the health risk of chemicals. Want to find out how many servings of a particular fruit or vegetable you could eat and still not have any adverse effects from pesticide residues? Check out the Pesticide Residue Calculator on the Safe Fruits and Veggies website. It turns out an adult woman would have to eat 13,204 servings of blueberries or 4,159 servings of conventional lettuce or 3,344 servings of organic lettuce in one day without any effect, even if these had the highest pesticide residues level ever recorded by USDA for blueberries or lettuce. For more information about fruits and vegetables and delicious ways to enjoy them, check out the Produce for Better Health Have A Plant website. Over 90% of people in the U.S. don’t eat enough fruits and vegetables so we should not be doing anything to discourage folks from enjoying any type of produce they like to eat, whether it is conventional, organic, fresh, frozen, canned, dried or juice. They all count toward your daily recommended fruit and veggie intake, are nutrient-rich and make you look and feel good. So, relax and enjoy the taste and fun of filling half your plate with fruits and vegetables. |
Neva CochranMS, RDN, LD, FAND Archives
November 2022
BlogsStay Safe at the Plate this Thanksgiving
The Real Truth about MSG: Myths, Science, Guidance An Aspiring Registered Dietitian: Advocating for Farmers, Consumers and Nutrition Strategies that Benefit Both Banned from Amazon: My DASH Diet for Dummies Review! Healthy Eating Resolutions You're Sure to Keep Same Song, Second Verse: The Dirty Dozen is Still a Dirty Lie Juice Can Go Back on Your Table Frozen Berries: Nutritious, Delicious and Safe to Eat The Lowdown on Lettuce and Listeria The Dirty Dozen is a Dirty Lie It’s in the CAN: Convenient, Affordable and Nutritious Meals When it comes to beer, choose taste not fear A Look at the EAT-Lancet Report: Can a Near-Vegan Diet Save the Planet and Feed the World? Peeling Back the Facts on Potatoes: Don’t Sack ‘Em Diet, Lifestyle and Diabetes: The SmartBrief headline that was really dumb Romaine Can Go Back on Your Plate |